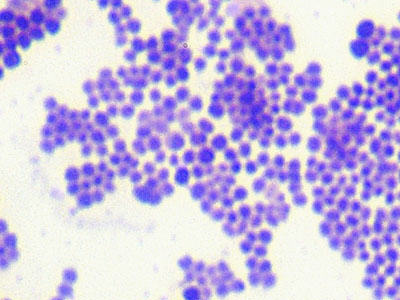
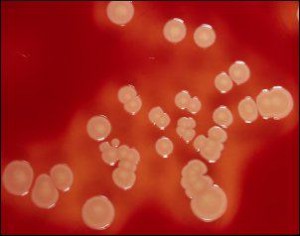
It takes about 1-6 hours after exposure to the bacteria for illness to become evident, and symptoms commonly include:
- Nausea
- Vomiting
- Diarrhea
- Loss of appetite
- Severe abdominal cramps
- Mild fever
The symptoms usually last about 24-48 hours and then resolve on their own with no additional treatment beyond drinking as much fluid as possible and resting in order to prevent dehydration. If the vomiting and/or diarrhea are so severe as to prevent hydration, then medical attention is necessary.
The prevention of food borne staph infections is similar to the prevention of any food borne infection and includes the following steps and precautions:
- Wash hands and under fingernails vigorously with soap and water before handling and preparing food.
- Do not prepare food if you have a nose or eye infection.
- Do not prepare or serve food for others if you have wounds or skin infections on your hands or wrists.
- Keep kitchens and food-serving areas clean and sanitized.
- If food is prepared more than two hours before serving, keep hot foods hot (over 140° F) and cold foods cold (40° F or under).
- Store cooked food in a wide, shallow container and refrigerate as soon as possible.
Antibiotic Resistance
As has occurred with many other species of bacteria, some Staph bacteria strains have developed resistance to commonly used antibiotics and have become increasingly difficult, if not impossible, to treat. As a group, these strains are referred to as methicillin-resistant-staphylococcus aureus or MRSA for convenience. Methicillin is a penicillin-type antibiotic that is used as a marker for wide-ranging resistance since once resistance to it occurs, it is likely that the strain will be resistant to many other antibiotics, although the extent of the resistance must be determined in a competent microbiological laboratory on a strain by strain basis. Increasingly, some strains of S. epidermidis have demonstrated similar resistance capabilities, increasing the risk that infections with that species could become more significant.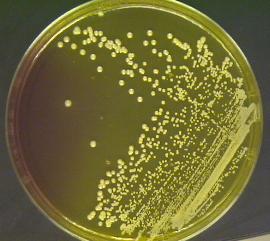
Community Acquired Infection
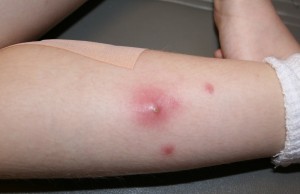
These types of resistant bacteria and the infections they cause were once only found in healthcare settings, but over the past years, such infections increasingly occured in otherwise healthy members of the community. Therefore, these cases are referred to as community acquired MRSA, or CA-MRSA. This new threat is very serious and widespread. The infection is spread by person-to-person contact, but since these bacteria can live on surfaces, including fabrics, for up to a month or more, environmental exposure cannot be ruled out as a route of infection. The vast majority of CA-MRSA cases involve skin infections that cause abscesses or other skin lesions. These often require surgical drainage by a healthcare professional and under no circumstances should a person attempt to drain a suspected MRSA lesion or abscess on their own as this could very likely cause the infection to spread and become much more severe. If in doubt, always consult a healthcare professional.