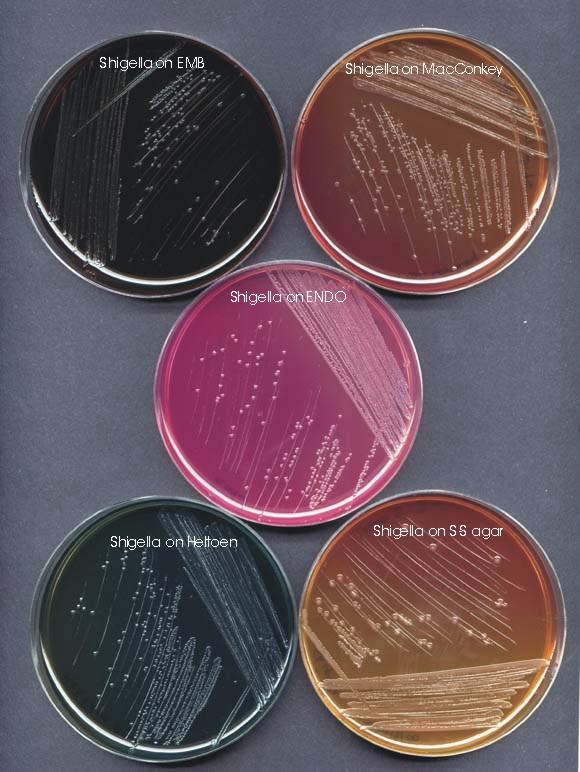
Shigella is a genus group of bacteria that contains four species, S. dysenteriae, S. flexneri, S. boydii, and S. sonnei. While these are frequently referred to as “species,” it is probably more scientifically correct to refer to them as biotypes of Escherichia, but because of the important medical differences between infections with Shigella versus most Escherichia the naming convention remains. As is also true of Salmonella species, there are numerous serotypes found within the different Shigella species, with the notable exception of S. sonnei which has only one serotype. Serotyping is important for scientific, especially epidemiological, studies, but is not likely to be relevant to most people.
Basic Shigella Statistics
S. sonnei is by far the most common Shigella species isolated in the United States, with most of the balance accounted for by S. flexneri. While Shigella infection is not uncommon in the United States, with almost half a million cases reported and undoubtedly, for various reasons similar to the situation with Salmonella, many more go unreported and/or unrecognized. Roughly 20% of cases in the United States are the result of international travel. Fortunately, in the United States at least, Shigella is not likely to be deadly, with only about 70 fatal cases reported yearly.
Dysentery
While the differences among the Shigella species are mostly academic, it could be important to recognize that S. dysenteriae is the causative agent of the disease bacterial, as opposed to parasitic, dysentery. In the developing world, and formerly in the United States as well, dysentery was a major killer, especially of children, and the disease often occurs in epidemic form. Great care must be taken with food and, especially water, when traveling in parts of the world where dysentery occurs, especially if an outbreak is in play at the time of travel. Consult a physician who specializes in travel medicine, or refer to the CDC travel pages for additional information about the risks of, as well as prevention steps for, dysentery. Classic dysentery is very uncommon in the United States today.
Transmission Settings
Most cases of Shigella occur in children. Almost all cases of Shigella are the result of person-to-person transmission of infected material, although it is possible for food and/or water to be infected if handled or served by an infected person. There is no animal, aside from large primates that are not native to the United States, or plant reservoirs of Shigella infection. Infection is most common in settings where hygiene is limited, especially in institutional settings, most notably in childcare settings, but prisons are also a location frequently plagued by poor hygiene and resultant epidemic outbreaks of infections such as Shigella.
Children and Shigella
Children are not known for their attention to hygiene, most importantly hand washing, and frequency of infection among children is likely due to their tendency to put things into their mouths that are likely to be contaminated by fecal material from infected children. Shared toys and surfaces are great reservoirs of Shigella infection commonly found in childcare settings. Childcare staff must also be aware of the risk to themselves, as well as to their families, and must practice diligent and effective hand washing, as well as considering disinfection of their households and workplaces on a regular basis as a means of prevention as families of small children, especially those who attend daycare, are considered at very high risk for infection with Shigella.
Symptoms of Shigella Infection
Shigella usually causes a gastrointestinal disease characterized by diarrhea, fever, and stomach cramps that start 1-2 days after infection. The diarrhea is frequently bloody, although the presence of fecal blood is not diagnostic for Shigella infection, nor does the absence of blood in the stool rule out Shigella infection. Culture of the stool is the only reliable way to diagnosis Shigella infection, and any competent microbiological laboratory should be able to isolate and identify Shigella bacteria. Many cases go undiagnosed because people don’t always seek medical care for diarrhea, and those that do often balk at the required collection of stool to make a Shigella diagnosis.