Escherichia Basics
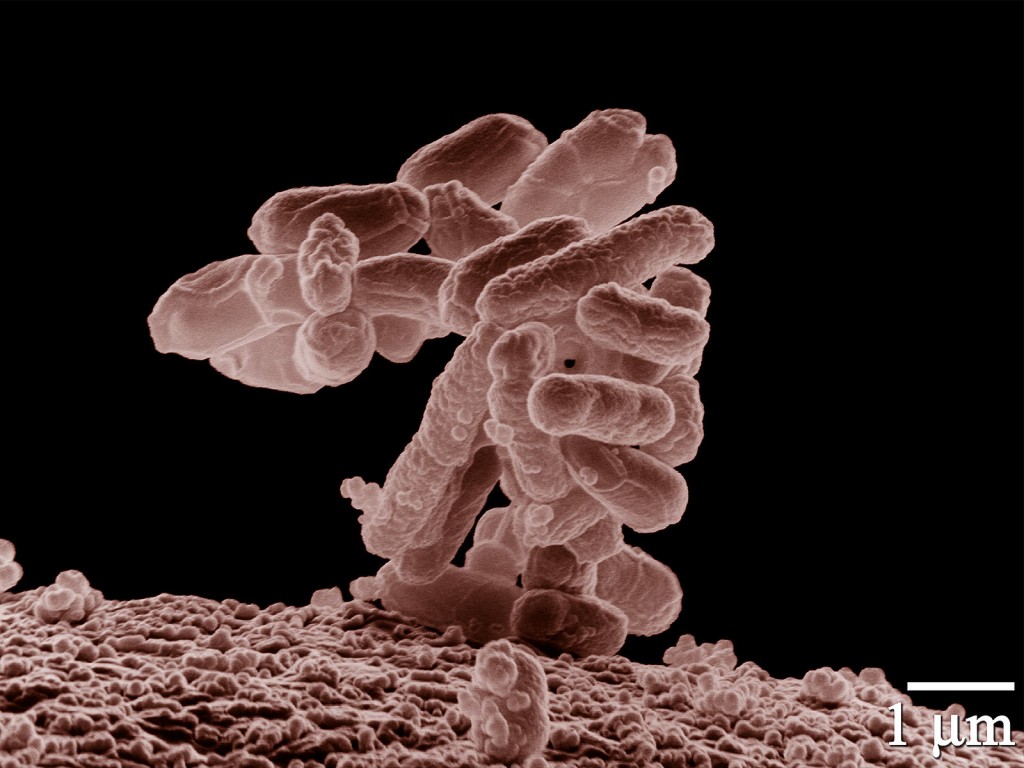
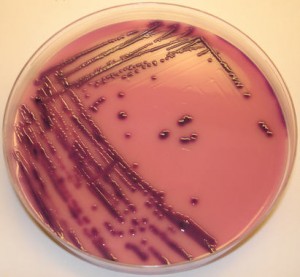
Escherichia is the genus name of a group of bacteria that contains at least 7 different species, although by far the most well-known and well-studied is clearly Escherichia coli (E. coli). Because E. coli is so common in the environment and in humans, as well as in other animals and because it is so easy to propagate (under the right conditions it will reproduce in as little as 20 minutes) is among the most well understood and manipulated of all the bacteria. When speaking of E. coli, one is speaking in generalities since there are hundreds of strains of E. coli which vary significantly, but not significantly enough for them to be considered separate species. The differences among the strains are important because while most E. coli are harmless, provided they remain in their normal environment of the gastrointestinal tract, some strains are quite virulent and can even prove fatal, even in otherwise healthy individuals. Fortunately, these extreme outcomes are rare.
Normal Bacteria
E. coli, under normal circumstances, is a normal and harmless inhabitant of the human intestinal tract. As long as E. coli are behaving as “normal flora” they can be important contributors to our intestinal and overall health. E. coli may assist in the digestion of nutrients and the elimination of waste material. And, as long as regular and harmless bacteria such as E. coli usually is, are occupying intestinal space, it makes it more difficult for harmful species, such as Clostridium difficile, to cause infection and illness.
Antibiotic Basics
Normal E. coli are very vulnerable to the overuse and misuse of antibiotics. Antibiotics, when misused, can cause serious illness. It is critical that antibiotics be used properly and completely and only used when prescribed by a physician and dispensed by a qualified pharmacist. Buying antibiotics on our own is a generally bad idea. It is most important to be certain that the cause of your illness is actually bacterial, not viral, as antibiotics are useless against viral infections. Perhaps needless to say, buying drugs on the Internet is almost always a bad idea and may, in fact, be illegal.
Pathogenic E. coli
While the vast majority of E. coli are harmless when limited to the intestinal tract, these bacteria are a major and common cause of infections, particularly of the urinary tract, even among non-hospitalized individuals, especially women. E. coli also commonly causes wound and other body site infections, including blood-borne systemic sepsis infections among patients in the healthcare-setting, including long-term care facilities. These types of infections are known as nosocomial, meaning they were acquired in the hospital or a related facility. Such infections are most common in people who have been institutionalized for a long period of time, who have indwelling devices such as blood or urinary catheters, and who are debilitated by other illnesses and/or advanced age.
The Emergence of Resistance
The majority of true infections caused by E. coli used to be easily resolved with common antibiotics, but as has been the case with many organisms in recent years, E. coli has developed resistance to varying degrees, depending on the strain, to many common antibiotics, most worryingly against the beta-lactam group of antibiotic medications. Such resistance is almost certainly due to the widespread overuse and misuse of powerful antibiotics by physicians who do not choose to wait to find out the actual cause, and most conservative effective treatment of, infections and illnesses, instead reaching for a sledgehammer when a much smaller tool would be as effective and safer. The proper diagnosis of infection and the careful and correct selection of treating antibiotics is ESSENTIAL to avoid further resistance developments. Competent microbiological analysis will easily detect infections with E. coli and will also identify the most effective and conservative means of treating the infection. Before taking antibiotics yourself or before giving them to loved ones, talk to your physician about such testing to ensure the effectiveness and safety of the proposed treatment. Results are typically available in as little as one to two days and in most cases this delay will not prove problematic.
Even in emergencies where treatment must start immediately, it is critical to follow up with microbiological testing to ensure that the given treatment is correct and conservative.